VOLUNTARY EXERCISE AFTER SPINAL CORD INJURIES: EQUIPMENT AND PROCESS THAT DEVELOPS AND SUSTAINS FITNESS AND HEALTH

By Mark S. Nash, Ph.D., FACSM, FASIA
Declining health and fitness are commonly known to accompany spinal cord injuries and disorders (SCI/D). Physical deconditioning and weakening of the upper limbs make essential daily activities such as wheelchair propulsion and body transfers more difficult to perform, thus challenging the activity and independence that persons with physical disabilities require throughout their lives. During the past few decades, attention has also focused on so-called cardiometabolic risk factors, including five critical health hazards: overweight/obesity, insulin resistance, hypertension, and lipid abnormalities. Evidence now suggests that these health risks appear soon after discharge from initial rehabilitation, tend to cluster, and in doing so represent more severe health hazards. They are also more challenging for stakeholders with SCI/D, their caregivers, and health care professionals to manage within the first year of living with a SCI/D and after that throughout their lifespans.
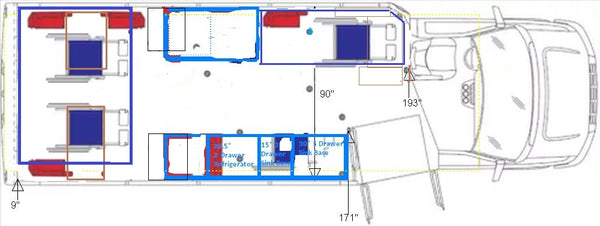
Current health guidelines designed for persons with SCI/D all recommend incorporating physical activity to a level permitted by their ability. Outdoor exercise is an option to fulfill this need. However, it may expose the individual to temperature extremes and uneven rolling surfaces that risk a fall from the wheelchair and ensuing injury. Thus, recent evidence suggests that home-based exercise is preferred for those with SCI. Home-based exercise also circumvents exercise barriers involving transportation, lack of physical access, and exercising in facilities that serve, have staff trained for, and use equipment designed for persons without a disability.

Equipment that satisfies the broad health needs of persons with SCI/D is challenging to find. Selected specialized exercise systems have used surface electrical stimulation to initiate the contraction of paralyzed muscles located below the injury level. These muscle contractions can be sequenced under microprocessor control to create purposeful movement such as cycling, although generally with poor motor efficiency and coordination. These electrically stimulated devices often exclude persons with injuries below the T10 spinal level and require special medical clearance and ongoing supplies such as electrodes and wire leads. Those with injuries and disorders that spare their sensation often find the electrical current uncomfortable, if not painful. While generally considered safe for home use, there is a need for electrode placement before each session. Risks of use include lower extremity fracture or bouts of autonomic dysreflexia. Importantly, there is limited transfer of lower extremity electrically stimulated exercise to benefit upper limb conditioning. It has long been clear that voluntary contractions of muscles above the injury level result in higher physical conditioning levels, and better risk reduction for cardiometabolic disease.
The arm crank ergometer has been a longstanding staple of upper extremity exercise for those with SCI/D. Essentially a table or platform mounted arm cycle, the device typically uses a rudimentary forward propulsion motion against resistance, with the upper limbs propelling the device while 180 degrees out of phase with one another. Few arm crank devices allow adjustment of the axis of rotation, meaning there is one set length for motion. Even fewer devices allow reverse propulsion against resistance. The continuous forward cranking imposes imbalanced forces that condition and tightens the anterior shoulder and chest while not similarly benefitting the posterior shoulder. The imbalance of the anterior and posterior shoulder actions may represent a cause of shoulder pain for persons with SCI/D. As the upper limbs of persons with SCI/D are essential for maintaining daily activities, the pain caused by cycle ergometry may exceed the benefit of physical conditioning.
To meet the complex needs of upper extremity conditioning without the hazards imposed by standard arm ergometry, the newly upgraded and technologically advanced Vitaglide better serves as an exercise mode after SCI/D. The device is a reciprocating ergometer with the arms moving near horizontally instead of in a cyclical pattern. The movement of the limbs are balanced between a forward pushing motion on one side of the body and a pulling action on the other side. In this way, the device maintains the anterior and posterior muscle balance for conditioning of the chest, shoulders, and back. Its features also permit synchronous rowing where both limbs move together in the same forward and backward direction. Unlike a cycling ergometer, the resistance for each arm can be set independently and spans work intensities that will develop both endurance and strength. The side arms allow the user to determine their preferred range of exercise motion instead of the device.
The Miami Project to Cure Paralysis at the University of Miami Health System has used the Vitaglide for several years as part of our comprehensive SCI/D lifestyle program and has been preferred by our program participants, so much so that they seldom use our cycle ergometers. The individualized resistance adjustment permits us to select optimum exercise intensities when the strength and endurance of the arms may be unequal. We have also found it easier to customize exercise programs and maintain records of performance incorporating time and work performed. Our ultimate goal is to encourage health-sustaining physical activity after SCI/D without injury.
Dr. Mark S. Nash is Associate Scientific Director for Research, Miami Project to Cure Paralysis, University of Miami Miller School of Medicine.